Routine assessment of Patient-Reported Outcome Measures (PROMs) in the DiaPROM trial
Hernar, Ingvild; Graue, Marit; Strandberg, Ragnhild Bjarkøy; Nilsen, Roy Miodini; Rekdal, Magne; Cooper, John; Løvaas, Karianne Fjeld; Madsen, Tone Vonheim; Tell, Grethe S.; Haugstvedt, Anne
Lecture
Accepted version
Åpne
Permanent lenke
https://hdl.handle.net/11250/2643675Utgivelsesdato
2019Metadata
Vis full innførselSamlinger
- Import fra CRIStin [3628]
- Institutt for helse- og omsorgsvitskap [2858]
Originalversjon
Hernar, I., Graue, M., Strandberg, R. B., Nilsen, R. M., Rekdal, M., Cooper, J., … Haugstvedt, A. (2019). Routine assessment of Patient-Reported Outcome Measures (PROMs) in the DiaPROM trial. Poster presentert ved Nasjonal diabetes forskningskonferanse og diabetesforum 2019, Gardermoen, Norge.Sammendrag
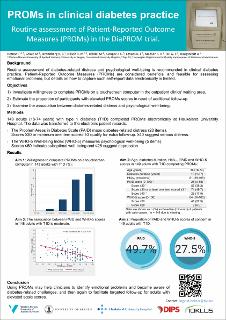
Objective: We aimed to investigate willingness to complete patient-reported outcome measures (PROMs) on a touchscreen computer in the outpatient clinics’ waiting area, estimate the proportion of participants with elevated scores in need of further follow-up, and examine the association between diabetes-related distress and psychological well-being. Methods: We recruited 149 adults (18-74 years) with type 1 diabetes to complete PROMs on a touchscreen computer at Haukeland University Hospital’s diabetes outpatient clinic. We used the Problem Areas in Diabetes Scale (PAID) and the WHO-5 Well-being Index (WHO-5) to examine diabetesrelated distress and psychological well-being. A PAID score ≥40 suggest serious diabetes-related emotional problems whereas a score of ≥30 or minimum one item scored ≥3 qualify for extra follow-up. WHO-5 scores ≤50 indicate suboptimal psychological well-being and scores ≤28 suggest depression. Results: One-hundred twenty (80.5%) participants were to at least a large degree willing to complete PROMs electronically. PAID scores of concern were reported by 74 (49.7%) participants, of which 26 (17.5%) scored ≥40. Forty-one (27.5%) reported suboptimal well-being, while nine (6.0%) reported scores suggesting likely depression. We found a moderate correlation (rho = 0.48, P <.001) between increased diabetes-related distress and reduced psychological well-being. Conclusion: The majority of participants reported willingness to complete electronic PROMs in the outpatient waiting area. Half of them reported moderate to serious diabetes-related distress and about one-fourth reported suboptimal psychological well-being. Using PROMs may help clinicians to identify emotional problems and to become aware of diabetes-related challenges and thus to facilitate targeted follow-up in forthcoming studies.